Hantavirus does not make headlines every week, but when it does, people pay attention fast. It is a rare but serious illness that comes from contact with infected rodents, and the gap between exposure and knowing you have a problem is wide enough to catch people completely off guard.
Having a good amount of knowledge about how hantavirus spreads could prepare you to take caution and avoid a genuine health risk. We did solid research, scrolled through lots of forums, and created a full picture, from what the virus actually is and how transmission works, to a clear and actionable hantavirus prevention framework you can apply at home, at a campsite, or anywhere rodents are likely to be present.
Table of Contents
What Is Hantavirus and Why Is It Rare?

Hantavirus is not a single virus. It is a family of viruses carried by rodents that can cause serious illness and death in humans who come into contact with infected animals or their waste. The two primary diseases it causes are hantavirus pulmonary syndrome, known as HPS, and hemorrhagic fever with renal syndrome, known as HFRS.
More than 40 species of hantavirus exist in nature, divided broadly into Old World and New World categories.
- Old World hantaviruses are found mainly in Europe and Asia and tend to cause bleeding disorders and kidney dysfunction.
- New World viruses, more common in the Americas, cause pulmonary edema, a condition where fluid builds up in the lungs and breathing becomes critically compromised.
The reason hantavirus stays rare despite how widely rodents are distributed comes down to transmission efficiency. The virus transmits rather poorly between species, and even in areas where a quarter of the local rodent population tests positive, annual human cases remain in the single digits. That relative inefficiency is the main reason the virus has not become a widespread public health crisis, though it does nothing to reduce the danger for the individuals who do get infected.
How Does Hantavirus Spread?

How hantavirus spreads is the most important thing to understand before anything else in this guide, because the transmission routes are specific and largely avoidable once you know what they are.
The primary route is aerosol transmission. When rodents infected with hantavirus urinate, defecate, or shed saliva in an enclosed space, those materials dry out and become dust. When a person disturbs that dust by sweeping, vacuuming, or simply moving through the space, they inhale microscopic particles carrying the virus directly into the lungs. This is how the majority of US hantavirus cases occur, and it explains why enclosed spaces like cabins, garages, sheds, and barns carry higher risk than open outdoor areas.
Rodent urine and deer mouse droppings are the most consistently identified sources in US cases. The deer mouse is the primary carrier of Sin Nombre virus, the most common hantavirus strain causing HPS in the United States, and it is found across virtually the entire country with the highest concentrations in rural western states.
Direct contact is a secondary route. A bite or scratch from an infected rodent can transmit the virus, as can handling rodents without gloves or touching your face after contact with contaminated surfaces. Eating food that has been contaminated by rodent droppings is another documented but less common route of infection.
Person-to-person transmission is almost nonexistent with one notable exception. The Andes virus, found primarily in South America, is the only known hantavirus strain capable of spreading between humans, and even that transmission is limited to people in very close contact with someone who is already seriously ill.
Every other hantavirus strain, including all strains circulating in the United States, does not spread from one person to another. A recent cluster of cases on the MV Hondius, a Dutch polar expedition vessel traveling from Argentina toward the Canary Islands, drew significant attention precisely because Andes virus involvement raised questions about shipboard spread.
The World Health Organization assessed the general public risk as low, a conclusion that aligns with what researchers consistently observe about how poorly hantavirus transmits even under favorable conditions. You definitely should know how hantavirus spreads through these specific routes cause it would later let you prevent the spread.
Hantavirus Signs and Symptoms
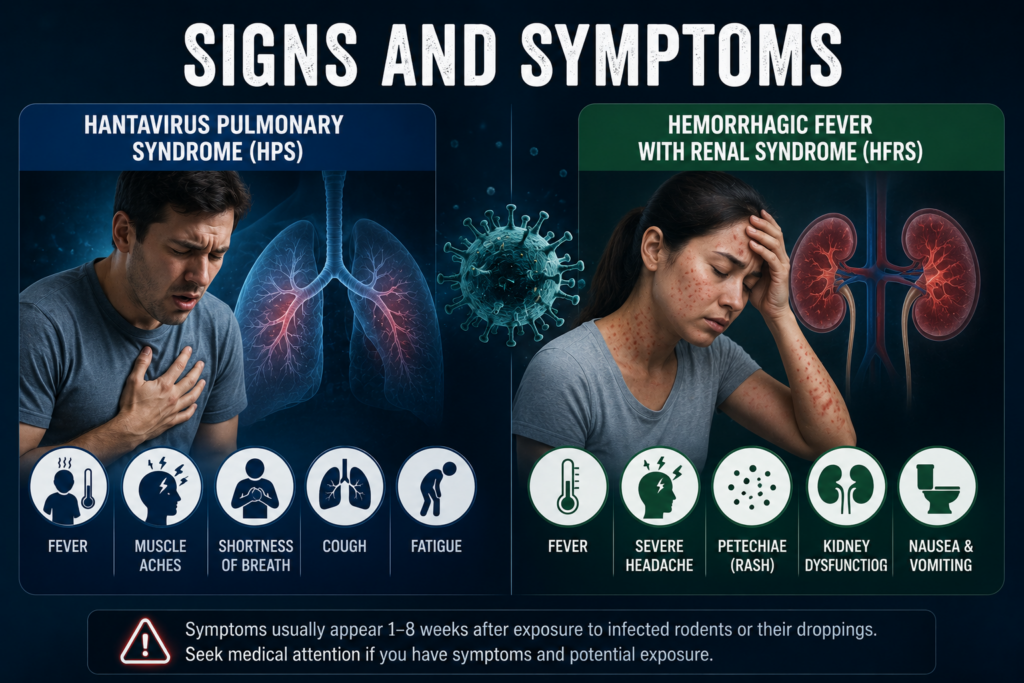
Hantavirus Pulmonary Syndrome
HPS is the form of hantavirus disease seen in the Western Hemisphere, including throughout the United States. Symptoms typically appear at least one week after exposure but can take up to eight weeks to develop, which makes tracing the source of infection genuinely difficult.
The early symptoms are flu-like and easy to mistake for something far less serious. Fever, chills, fatigue, and muscle aches in the large muscle groups, particularly the thighs, hips, back, and sometimes shoulders, are the consistent early signs. About half of all HPS patients also experience headaches, dizziness, and more pronounced chills. Many develop abdominal pain, nausea, vomiting, or diarrhea in this initial phase.
Four to ten days after those early symptoms appear, the situation can deteriorate rapidly. Cough and shortness of breath develop and can worsen quickly, leading to critical respiratory failure as fluid fills the lungs. Among patients who reach this respiratory stage, approximately one-third do not survive. Early symptoms identified quickly and treated aggressively in an intensive care setting represent the best available path to survival.
Hemorrhagic Fever with Renal Syndrome
HFRS is caused by hantaviruses found primarily in Europe and Asia, though Seoul virus, one of the strains responsible for HFRS, circulates worldwide including in the United States. Where HPS attacks the lungs, HFRS attacks the kidneys and the vascular system.
Symptoms of HFRS generally develop within one to two weeks of exposure, though in rare cases they take up to eight weeks to appear. Initial symptoms begin suddenly with intense headaches, back and abdominal pain, fever and chills, nausea, and blurred vision. Flushing of the face, inflammation or redness of the eyes, and a rash are common in the days that follow.
Later-stage symptoms include low blood pressure, acute shock from reduced blood flow, internal bleeding from vascular leakage, and acute kidney failure that can produce severe fluid overload throughout the body. The severity varies significantly depending on the specific virus. Hantaan and Dobrava virus infections are the most dangerous, with fatality rates between 5 and 15 percent. Seoul, Saaremaa, and Puumala infections tend to produce more moderate illness with fatality rates below one percent. Complete recovery from HFRS can take several weeks to several months.
How Common Are Hantavirus Infections in the US?
According to the Centers for Disease Control and Prevention, 864 laboratory-confirmed cases of hantavirus disease were reported in the United States from the start of surveillance in 1993 through 2022. Cases have turned up in 40 states, but the concentration is heavily weighted toward rural areas in the western United States, with California, Washington, Arizona, New Mexico, and Colorado accounting for a disproportionate share.
Globally, between 10,000 and 100,000 hantavirus infections are estimated to occur each year, with the majority concentrated in Asia and Europe. In the Americas, reported cases run between 150 and 300 annually, and Argentina, Brazil, Chile, and Bolivia typically account for most of those. The United States identifies between 15 and 50 cases per year, a number that reflects both genuine rarity and the likelihood that some milder cases go undiagnosed.
Does the Latest Outbreak Pose a Risk?
The MV Hondius cluster brought hantavirus back into international news in 2025, but the broader public risk assessment from the WHO and independent researchers remains consistent with the historical picture. The general public risk is low.
Steven Bradfute, an immunologist and hantavirus researcher at the University of New Mexico Health Sciences Center, noted that even in New Mexico where around a quarter of tested rodents carry the virus, the state still records only a handful of human cases annually. The virus transmits rather poorly, he explained, and even though the infections it does cause are dangerous, it is not positioned to become a widespread outbreak pathogen under normal circumstances.
The specific strain involved in any cluster matters considerably, both for predicting mortality rates and for understanding transmission dynamics. Ongoing surveillance and rapid strain identification remain the core tools public health systems use to assess and contain emerging clusters.
How Is Hantavirus Treated?
There is no specific antiviral drug approved for hantavirus. Treatment is supportive and focused on managing the symptoms as aggressively as possible. For HPS patients who develop respiratory failure, mechanical ventilation and careful fluid management in an intensive care unit are the standard approach. Oxygen therapy and dialysis are used as needed depending on the organ systems most affected.
Early recognition is the single most important factor in survival outcomes. Patients who are admitted to intensive care before full respiratory collapse occurs have significantly better survival rates than those who arrive later in the disease course. If you have had potential exposure to rodent droppings or rodent-infested spaces and develop fever, muscle aches, or breathing difficulties in the weeks that follow, tell your doctor about the potential exposure immediately so they can factor it into their assessment.
How to Prevent Hantavirus Infection
1. Rodent Control and Exclusion
Effective hantavirus prevention starts with reducing the rodent population in and around your living spaces. Set snap traps rather than glue traps in areas where rodent activity is suspected, because glue traps keep the animal alive and stressed, which increases the amount of virus-laden secretions released into the environment. Place traps along walls and in corners where rodents naturally travel. Check and clear traps wearing disposable gloves, and seal the animal in a plastic bag before disposal.
Seal entry points throughout your home’s exterior. Mice can pass through gaps the size of a dime, and rats through gaps the size of a quarter. Steel wool packed into gaps followed by caulk or hardware cloth provides a durable barrier that rodents cannot chew through easily. Pay particular attention to pipe entry points, foundation cracks, and gaps around utility lines.
2. Safe Cleaning of Rodent Droppings: Step-by-Step Protocol
Safe cleaning of rodent droppings is one of the most specific and important aspects of hantavirus prevention, and most people do it wrong the first time without realising the risk.
- Step one: Ventilate the space before you enter. Open windows and doors and allow fresh air to circulate for at least 30 minutes before beginning any cleaning activity. Step outdoors and let the ventilation do its work before you go back in.
- Step two: Put on rubber or plastic gloves and a properly fitted N95 respirator mask before touching anything. Eye protection is advisable in heavily contaminated spaces.
- Step three: Spray all droppings, nesting material, and contaminated surfaces with a disinfectant solution. A mixture of one and a half cups of bleach per gallon of water works effectively. Let it soak for at least five minutes before wiping.
- Step four: Use paper towels or disposable cloths to wipe up the moistened material. Never dry sweep or vacuum without a HEPA filter, as this launches aerosol particles directly into the breathing zone.
- Step five: Seal all waste material, gloves, and paper towels in a plastic bag. Double-bag it and dispose of it in an outdoor rubbish bin. Wash your hands thoroughly with soap and water after removing gloves.
3. Home Sealing and Ventilation Techniques
Sealing your home against rodent entry and maintaining good ventilation work together as a combined hantavirus prevention strategy. Fit door sweeps on all exterior doors and check that crawl space vents are screened with fine wire mesh. Keep firewood stored away from the house and at least 18 inches off the ground to take away ground-level harborage near the foundation.
Ventilate enclosed spaces regularly, particularly basements, crawl spaces, and attached garages. Stagnant air allows dried rodent waste particles to accumulate without dispersal, and a single heavily infested space can build up a meaningful aerosol risk over weeks or months.
4. Protective Gear and Best Practices
Mask protection is non-negotiable when working in spaces with known or suspected rodent activity. A standard surgical mask does not provide adequate filtration for viral aerosols. An N95 respirator properly fitted over the nose and mouth is the minimum appropriate protection. For work in heavily contaminated spaces, a half-face respirator with P100 cartridges provides stronger coverage.
Gloves should be worn whenever handling traps, cleaning droppings, or working in rodent-frequented spaces. Wash clothing worn during clean-up separately from household laundry, using hot water.
5. Cabin, Garage, and Campsite Specific Prevention
Closed-up cabins and seasonal properties that have sat empty through winter carry a disproportionate share of US hantavirus risk. Before entering a cabin that has been closed for weeks or months, open all windows and doors and allow thorough ventilation for at least 30 minutes before going inside. Do not sleep in a cabin that shows signs of rodent activity until the space has been properly cleaned and treated.
At campsites, avoid sleeping directly on the ground and keep food in sealed containers. Tents with sealed floors provide meaningful protection. If you are camping in areas with known high rodent populations, particularly in rural southwestern states, the prevention tips above around site selection and food storage take on added weight.
6. Long-Term Risk Reduction Framework
Sustained hantavirus prevention is not a single clean-up event. It is an ongoing practice built around regular inspection and maintenance. Check your home’s exterior twice a year for new gaps or damage that could allow rodent entry. Maintain snap traps in attics and crawl spaces as a monitoring tool even when active infestation is not suspected. Keep grass cut short around the property perimeter and take away debris piles that create harborage.
In high-risk areas, consider an annual inspection by a licensed pest control professional who can identify vulnerabilities you might miss. Document any rodent activity you find and address it promptly rather than waiting to see whether the problem resolves on its own.
May 2026 Situation As Per WHO at a glance

On 2 May 2026, a cluster of passengers with severe respiratory illness aboard a cruise ship was reported to the World Health Organization. The ship is carrying 147 passengers and crew. As of 4 May 2026, seven cases (two laboratory confirmed cases of hantavirus and five suspected cases) have been identified, including three deaths, one critically ill patient and three individuals reporting mild symptoms. Illness onset occurred between 6 and 28 April 2026 and was characterized by fever, gastrointestinal symptoms, rapid progression to pneumonia, acute respiratory distress syndrome and shock. Further investigations are ongoing. The outbreak is being managed through coordinated international response, and includes in-depth investigations, case isolation and care, medical evacuation and laboratory investigations. Human hantavirus infection is primarily acquired through contact with the urine, faeces, or saliva of infected rodents. It is a rare but severe disease that can be deadly. Although uncommon, limited human to human transmission has been reported in previous outbreaks of Andes virus (a specific species of hantavirus). WHO currently assesses the risk to the global population from this event as low and will continue to monitor the epidemiological situation and update the risk assessment.
Frequently Asked Questions (FAQs)
Can hantavirus spread from person to person?
With one known exception, hantavirus does not spread between people. The Andes virus found in South America is the only strain documented to spread person-to-person, and even that transmission is limited to close contact with someone who is severely ill. All strains circulating in the United States, including the deer mouse-carried Sin Nombre virus responsible for most US HPS cases, do not transmit between humans.
What kills hantavirus in droppings?
A bleach solution mixed at one and a half cups per gallon of water effectively kills hantavirus when applied to contaminated surfaces and allowed to sit for at least five minutes before wiping. Commercial disinfectants with an EPA registration for use against viruses also work. The critical step is wetting the material before any physical contact to prevent aerosol generation.
How common is hantavirus in specific states?
New Mexico, Colorado, Arizona, California, and Washington account for a disproportionate share of US cases. New Mexico in particular has documented high rates of infected deer mice in the environment, though human cases remain very low annually given that infected rodent population. Montana, Utah, and Texas also see regular case reports. Cases outside the western United States are considerably less frequent but have been confirmed in 40 states since surveillance began in 1993.
Is it safe to vacuum mouse droppings?
Vacuuming dry rodent droppings is one of the higher-risk actions you can take in a contaminated space. Standard vacuum cleaners aerosolize the dried material and blow it directly into the breathing zone of the person cleaning. A HEPA-filtered vacuum used with an N95 mask reduces but does not eliminate the risk. The correct approach is always to wet the droppings with disinfectant solution first and wipe them up manually, as described in the safe cleaning protocol above.
Do cats or dogs spread hantavirus?
Domestic pets do not spread hantavirus to humans. Cats and dogs can bring infected rodents into the home or disturb rodent nesting sites, which increases the indirect risk of human exposure to contaminated materials. The infection pathway still runs from the rodent waste to the human, not from the pet to the human. Keeping pets from hunting rodents in high-risk areas reduces that indirect exposure risk.










